Strategies to reduce COVID-19 infection and spread
Background: How to Live While COVID-19 is Spreading
The CDC is responsible for protecting the public’s health, yet it has largely abandoned collective and systemic measures to protect people from COVID-19. Instead, since May 2021, the CDC has gone against the foundations of public health that are based on principles of collective responsibility, health equity, and human rights by declaring “your health is in your hands.”
While the virus that causes COVID continues to spread, we learn more each day about the dangerous health effects that can come from COVID infection (and re-infection), even for mild cases, even for vaccinated people, even in young people, and even in people with no pre-existing conditions.
Now, individuals are almost solely responsible for preventing COVID infections, self-assessing their risk, and figuring out what protective steps to take, and when. Many key public health leaders and decision makers
now downplay the risk of infection, refusing to take action unless community spread increases hospitalizations.
Independent movement The People’s CDC opposes the abandonment of policies that are proven to reduce the spread of COVID. To help us all understand the vast amount of information (including disinformation) about COVID, the People’s CDC has prepared guidance based on scientific research about the protective measures we can use while the virus that causes COVID is still spreading.
We want you to have the best information about how to protect yourself and those around you from getting or spreading COVID. This resource is a practical guide for how to avoid infection while COVID is spreading and explains what layers of protection you can use to reduce the spread of COVID.
We Recommend Using Layers of Protection
Several proven tools will help keep us and others safer from COVID. We can think of these tools as layers of protection. If we use more layers to
protect ourselves and others, we are less likely to contract COVID—and the virus will have fewer opportunities to spread.
COVID is spread most easily through the air. These four layers of protection will make it less likely for COVID to spread:
- Improving indoor air quality.Wearing well-fitting, high-quality masks.Increasing physical distance.Reducing time spent close to others indoors.
You can also reduce your chance of catching or spreading COVID with these three layers of protection:
- Limiting the number of people you are around.Getting your vaccine and recommended boosters, which helps decrease your risk of death and other health issues if you do catch COVID.Testing to learn if someone has COVID, even if they don’t feel sick,
so they know to isolate and to seek treatment.
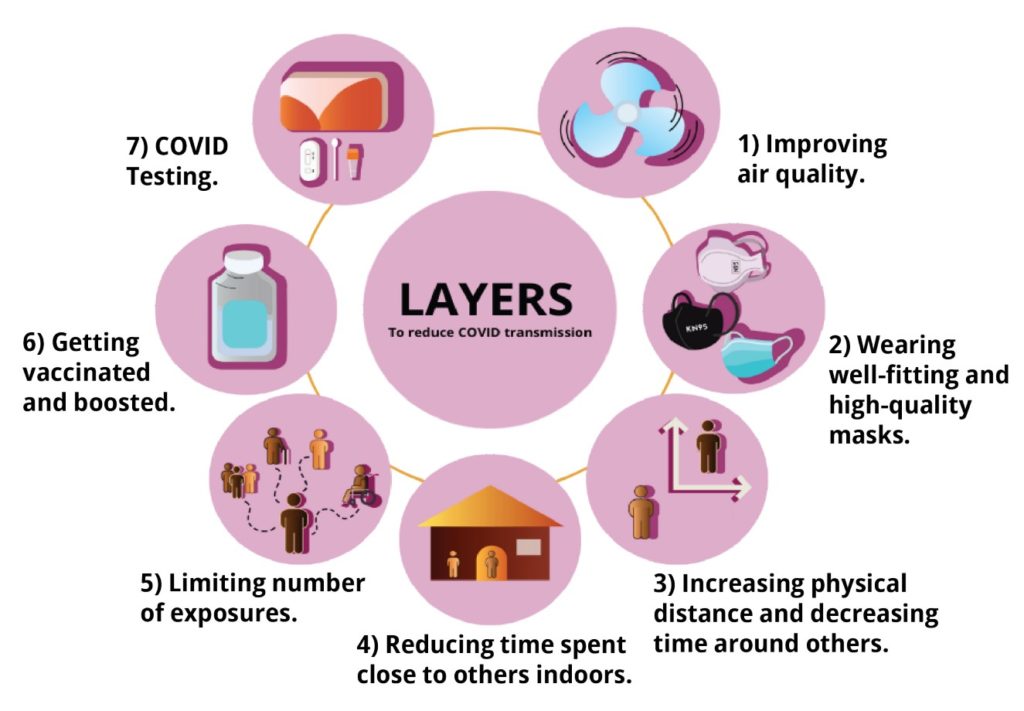
The Layers of Protection People’s CDC Recommends
1. Improving Indoor Air Quality
• Open windows for increased ventilation. Ideally, open windows on
different walls for cross ventilation.
• Indoor air quality can be improved with portable air purifying units with
HEPA filters or more affordable homemade versions of these, such as
Corsi-Rosenthal boxes. *
• Outdoors is the best ventilation!
*People’s CDC points out drawbacks to Corsi-Rosenthal boxes in Appendix 3 of our Document, Ventilation for Coronavirus in Schools.

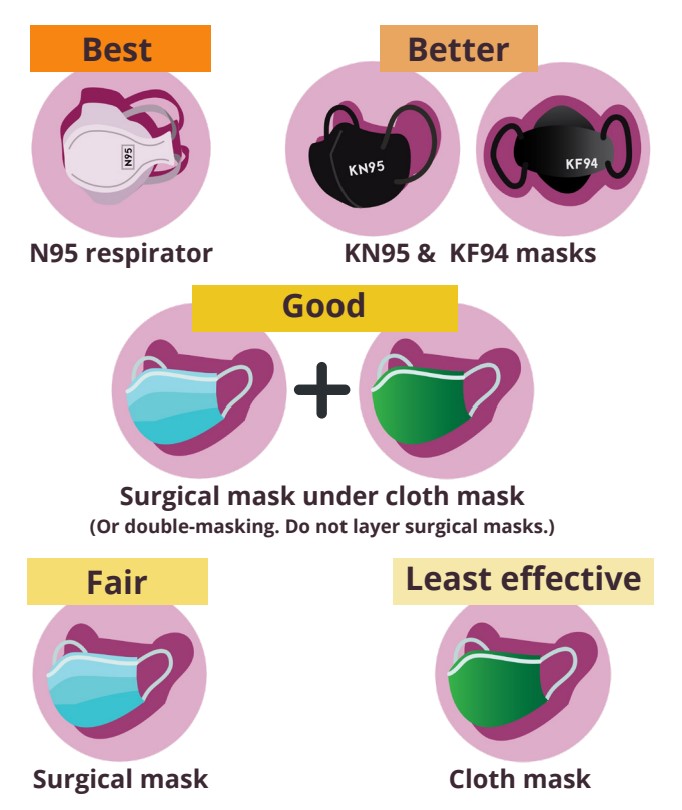
2. Wearing Masks: Well-Fitting and High-Quality are Key!
• The best well-fitting, high-quality masks to protect you and others
from COVID are N95, KN95 or KF94 masks, as these stop tiny
virus particles and droplets. Some N95s (also called N95 respirators) have a tighter fit because they have two straps that go over the head instead of ear loops.
• Masks worn correctly, covering the mouth and nose, help keep people from becoming infected with, or spreading, COVID.

3. Increasing Physical Distance
• If you increase the space between you and others, then you are exposed to less virus from an infected person breathing, talking, coughing or sneezing.
• It is often recommended you distance yourself 6 feet from others, but that guidance was based on a misunderstanding of how virus particles travel. Large droplets from coughing or sneezing do drop to the floor
after about 6 feet on average, but can travel much farther, depending on the forcefulness of the cough/sneeze and airspeed in the room.
• In an unventilated and unfiltered space, tiny particles of the virus (aerosols) can linger for hours in the air and spread throughout a space, and you can be exposed at any location in the space.

4. Reducing Time Spent Close to Others
• If we spend less time in spaces where there is potentially much virus in the air, then we breathe in less virus and lower our risk of infection.
• There is no specific number of minutes (or distance) that is proven to be safe indoors if unmasked.
• Examples of where there might be a lot of virus in the air are spaces where it is crowded, where people are close, and/or there is inadequate ventilation, including buses and trains, concert venues, and certain work
environments.
Unfortunately there is limited data on COVID spreading outdoors in crowds. While there is excellent ventilation, being close to others could still spread COVID.
5. Limiting the Number of People You Are Around
• If we are exposed to fewer people, then we are less likely to become
infected and potentially infect others.
• Because 40% of people with COVID have NO symptoms, it is very easy
to have COVID without knowing it and to spread it unknowingly when
around others.
This layer can be the hardest to control! We don’t always have a choice over how many people we interact with where we live, where we go to school or work, on the bus or other public transit, or elsewhere in the community. If you cannot reduce the number of people you are around, you can use the other layers of protection listed here that you can control.
6. Getting Vaccinated and Staying Current on Recommended Vaccine Doses
• The best prevention and protection against severe illness and death from COVID is to be up-to-date on your vaccines, which includes getting
your booster dose(s).
• People who are vaccinated and boosted can get COVID, but they rarely get seriously ill, have to be hospitalized, or die from COVID.
Some immunocompromised individuals, depending on disease or treatment status, have reduced protection from COVID vaccines. It is important to get booster shots available to immunocompromised individuals and use additional layers of protection discussed in this
document whenever possible.
7. Testing
• There are two main types of testing for COVID: Rapid Antigen (Ag) tests (sometimes called At Home tests or RATs) and PCR tests.
• Testing before gathering indoors and unmasked with people increases the chance of identifying asymptomatic cases.
• Use testing when experiencing symptoms to see if it is COVID.*
• People with COVID should test to exit isolation. Rapid tests can be used after a confirmed positive case to see if you are no longer infectious.
• You can test during quarantine (when you have been exposed to someone with COVID). During the 10 days following exposure, test to see if you have become infected.
• Some schools, businesses, and people test routinely to try to check if anyone has asymptomatic infection to prevent spread.
*If you test too soon after being infected, a PCR or rapid test may give you an incorrect result.

Where and When Do I Apply These Layers of Protection?
Contrary to CDC’s mostly individualist philosophy, the People’s CDC recommends regular use of these Layers of Protection while COVID is spreading, because the more we use these layers, the more we work together to stop spreading COVID.
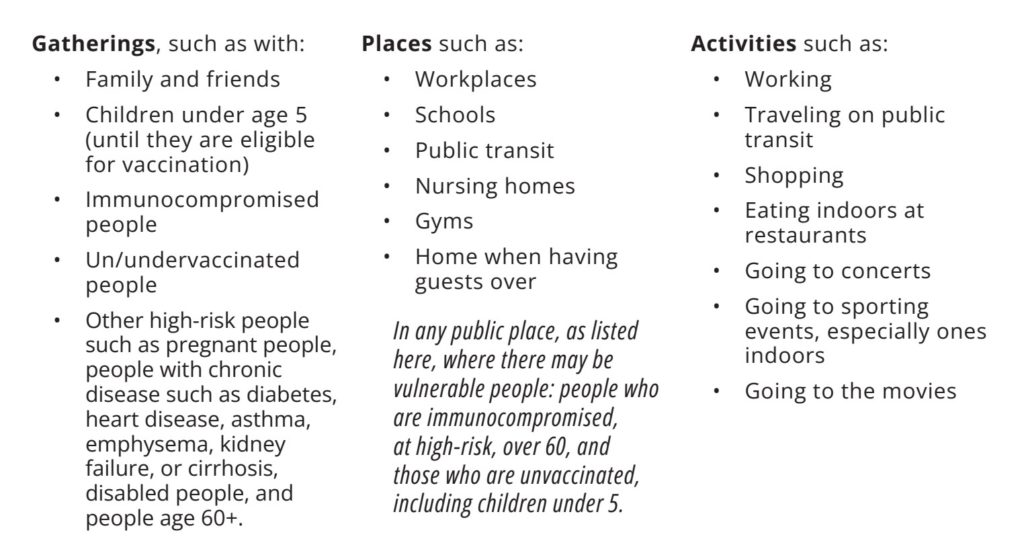
Here are examples of kinds of gatherings with people, types of places
and activities where we recommend you apply layers of protection. While
official government, school or business public health policies that support
protections against COVID transmission are weakening or disappearing, the People’s CDC encourages you to use these tools to reduce your chances of getting or spreading COVID in a variety of settings.

For more resources, including a weekly weather report on COVID in the United States, visit peoplescdc.org, Follow us on Twitter, and join our mailing list.
For more information check out the Layers of Protection pdf found below as well as other information on fighting COVID-19 throughout our website!