The Weather: We remain in a sustained COVID surge: every week since early June, 99% of US population lives in high or substantial transmission.
In fact we’ve updated our transmission map (h/t @JasonSalemi) to show how high transmission is, 73% living in the highest two levels!
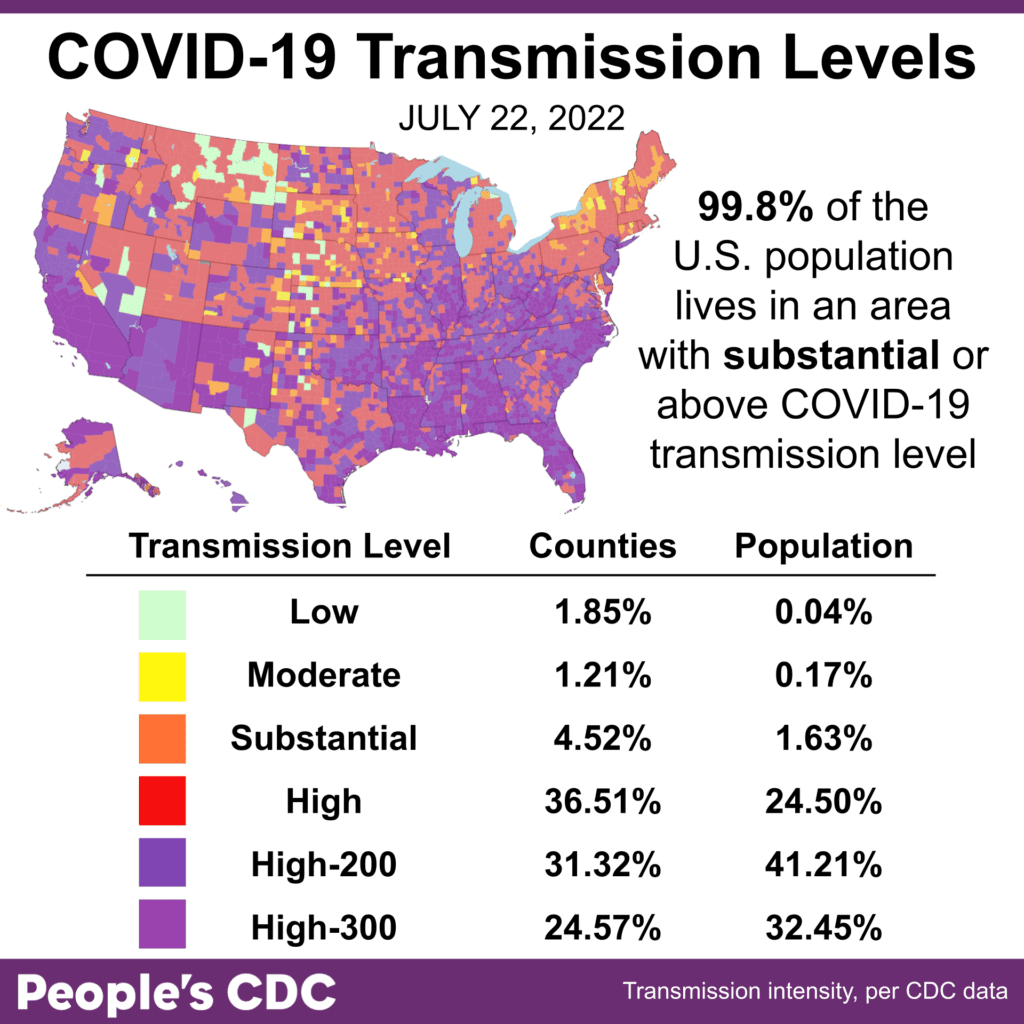
Watch the spread here: https://www.youtube.com/watch?v=QGsKEGL0bvg
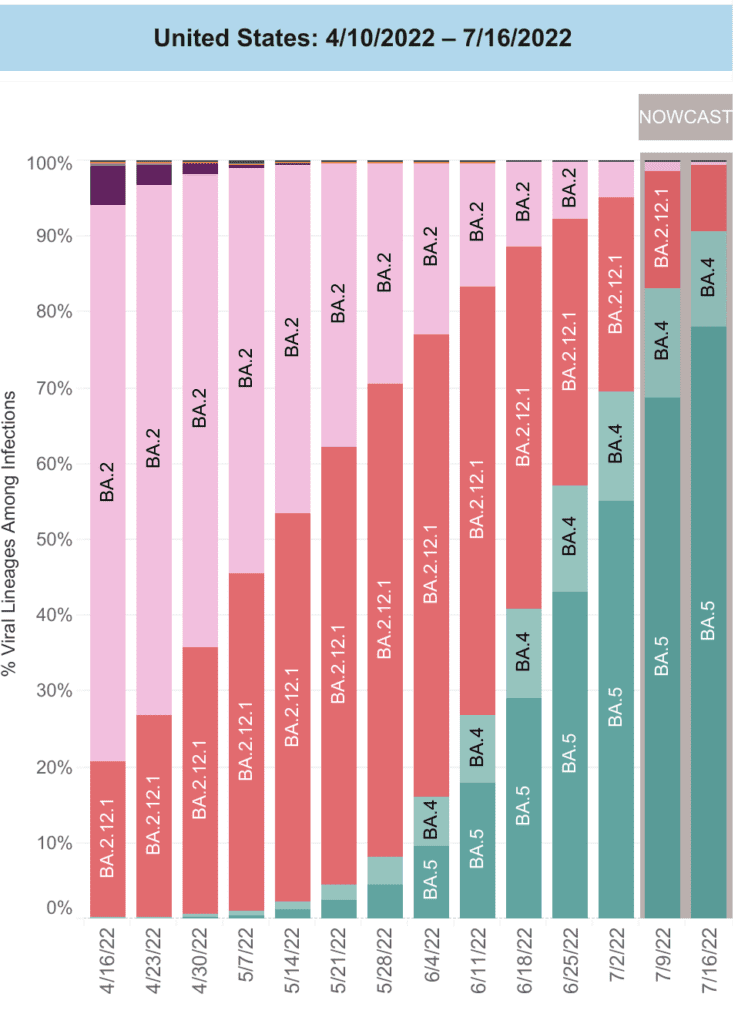
On Variants: While BA4/5 now make up 90% of cases nationally, no new variants are rising yet.
Centaurus (BA2.75) has been detected in some states but it is not clear if it will outpace BA5 – we’ll keep updating on this!
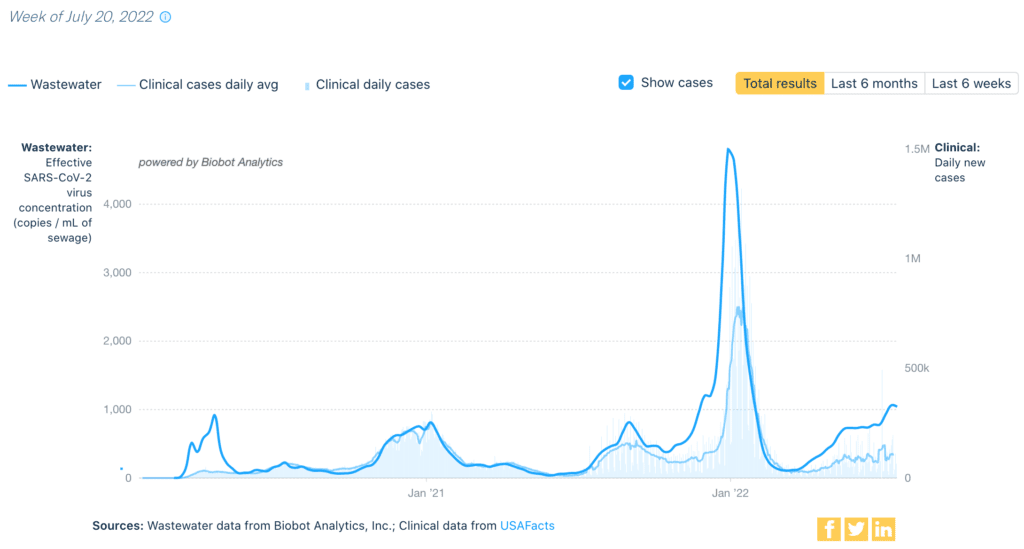
Wastewater Monitoring: National wastewater data from @BiobotAnalytics shows a small dip for the first time in months.
And yet, we are still at levels higher than any surge before Omicron. Levels are fluctuating, but remain high in all regions.
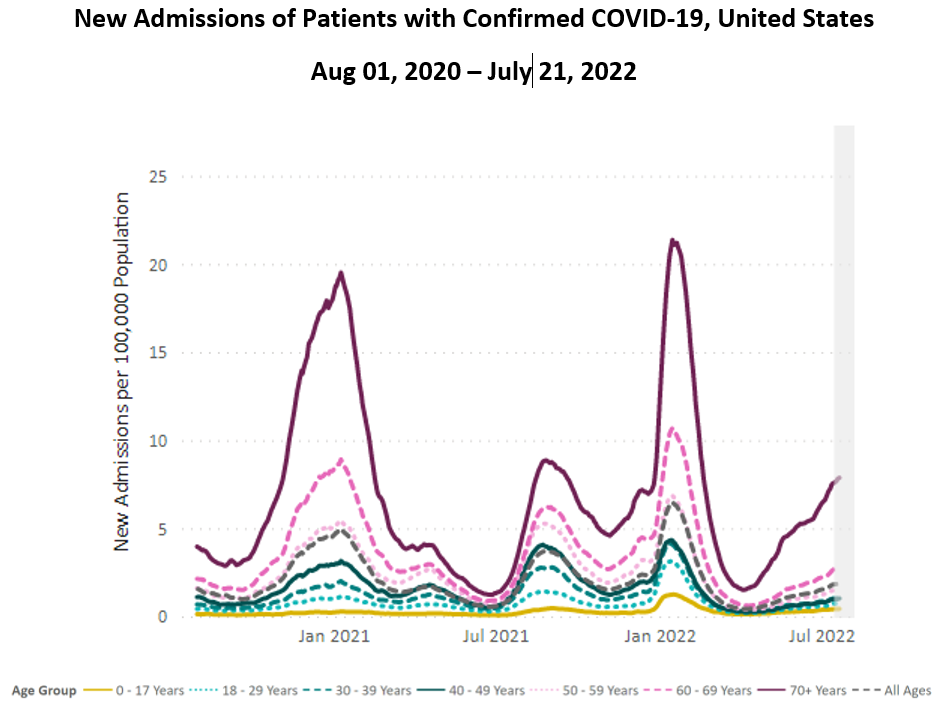
Hospitalizations: For 13 weeks in a row, hospitalizations are still rising nationally – with the most dramatic increases among those 70 and older.
This sustained surge is having significant health impacts on many living in the US – and is unsustainable for our healthcare workers.
Deaths: From July 14 to July 20, 2,468 people died of COVID nationally. Even the New York Times commented how this version of “normal” is brutal – and the estimate of 100,000 dead per year will almost certainly be exceeded this year.

![This is a paragraph of text from the editorial, with a highlighted sentence: “As a ballpark estimate, [Dr Trevor Bedford, an evolutionary virologist] says, going forward we can expect that every year, around 50 percent of Americans will be infected and more than 100,000 will die.”](https://bej.gbh.mybluehost.me/wp-content/uploads/2022/07/7.25.22_NYTPart2-1024x325.png)
Of course, sustained high levels of cases, hospitalizations & death are not inevitable. The government could choose a better response – updated vaccines, free high-quality masks & testing, improved ventilation, & paid sick leave – and create a better, healthier “normal.”
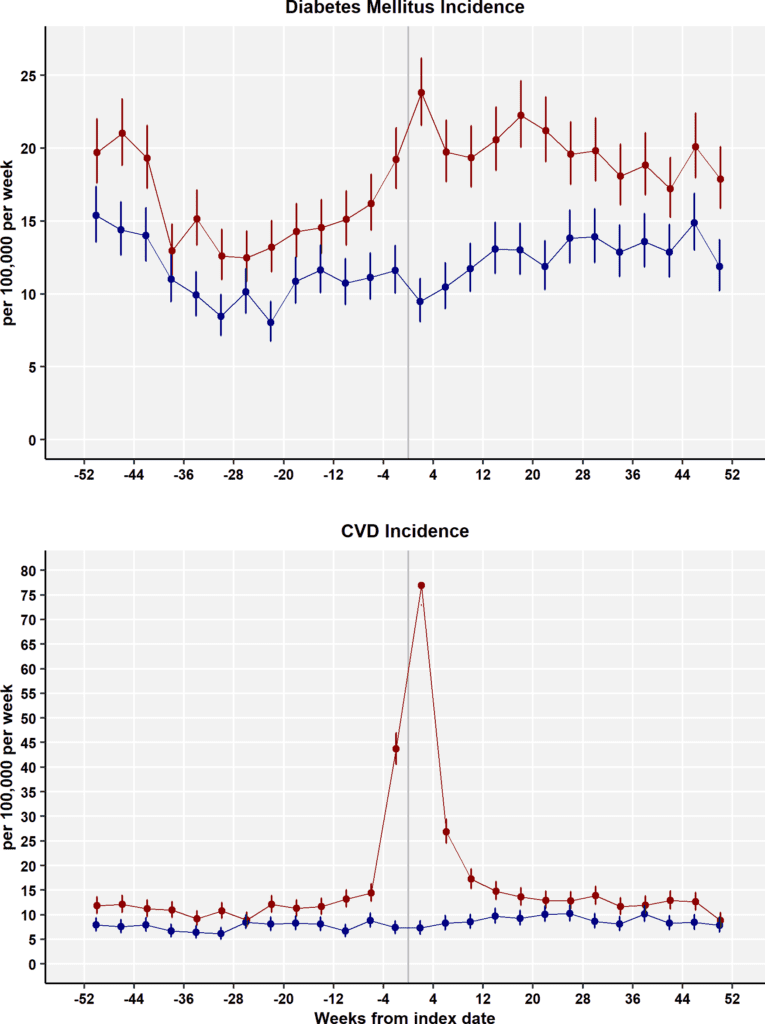
On Long COVID: Another study has confirmed higher diagnoses of diabetes and cardiovascular disease in the 4-12 weeks after a COVID infection. This suggests a need for increased monitoring during early recovery.
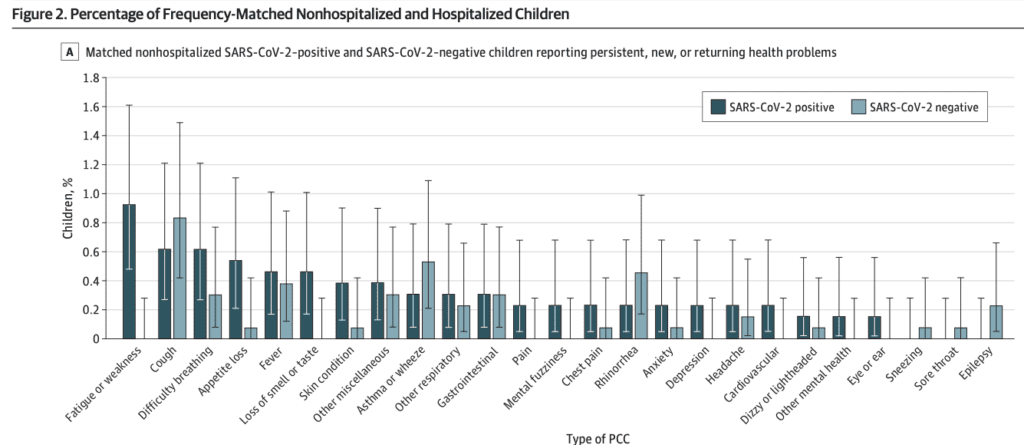
In one of the first cohort studies to examine children who were tested for COVID at ERs, and again at 90 days, 4.6% of COVID-positive children had new or persistent symptoms at follow-up, compared to only 2.7% in COVID-negative children.
These proportions nearly doubled in hospitalized children.
Additionally, the study identified symptoms that were more common in the COVID-positive children at follow-up, including: fatigue or weakness, loss of appetite, general psychological concerns, and continued loss of smell or taste.
Forecast: Existing boosters based on the original COVID (ancestral) strain may provide sufficient protection against severe outcomes from BA.5.
Everyone 5 and older is eligible for a booster; those over 50 or immunocompromised are eligible for a second booster!
LA County’s Public Health Director, Barbara Ferrer, stated re: mask mandates: “I don’t think we should be settling for high mortality that disproportionately affects people who have less economic means and people of color.”
She went on to state that “masking remains a strategy that layers in protections when transmission is high.”
Be Prepared: BA5 has rapidly outgrown all other variants in the US. We haven’t yet seen evidence of a new variant that can overtake it.
Although this may give us a brief break before the next variant emerges, repeat infections from BA5 could also keep cases high for the foreseeable future.
By reducing transmission, we give the virus fewer chances to adapt and keep each other healthier.
Layers of protections – high-quality masks, ventilation, vaccines, & testing – remain our best defense.
Sources – Check out the links throughout and see our website for more! https://bej.gbh.mybluehost.me
Apology
PCDC apologizes for our coverage of monkeypox (MPV) last week. Both PCDC volunteers and outside readers noted that our framing perpetuated some of the same errors of exclusion and bigotry we seek to oppose. We include the original language here for reference and accountability.* We’re currently reflecting on how we engage with the topic going forward. We aim to share information that is non-stigmatizing, accurate, and prioritizes those most impacted. If you have MPV resources you’ve found helpful, or thoughts on how PCDC can best contribute, please let us know via the form linked here.
